What does ICSI involve?
It is currently the most common In Vitro Fertilisation technique.
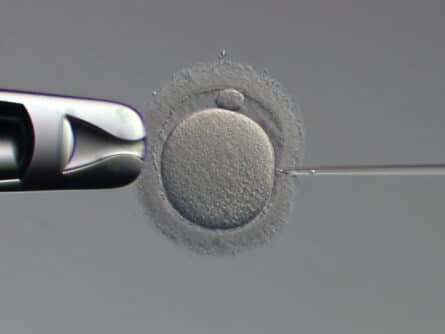
This is a technique in which a spermatozoid is injected into an egg with the help of a microneedle, compared to conventional fertilisation in which the eggs are surrounded by thousands of spermatozoids and kept under special conditions in order to help one spermatozoid reach the egg and fertilise it.
For your security and because of the advantages it offers, ICSI is used in practically all In Vitro Fertilisation cycles.
When is it recommended?
It is especially recommended in the following cases:
- Severe sperm abnormalities
- Poor egg quality
- Few or very valuable eggs
- Advanced maternal age
- Suspicion of poor fertilisation rates
- Cases of conventional IVF when fertilisation has not occurred
- Spermatozoids obtained by testicular biopsy
First fertility visit is free
Request your first appointment cost-free at the clinic closest to you
Frequently asked questions about ICSI
After the ovarian stimulation and egg retrieval, patients are advised to carry on with their usual activities but to stay relaxed and take it easy. Basically, the recommendation for the first day or day and a half is to avoid strenuous physical activity and exercise.
The process of conventional IVF is more natural than IVF-ICSI because the egg is left to incubate alongside the spermatozoids for a long period of time.
Usually, one spermatozoid will be able to bind to the zona pellucida of the egg, make its way inside and then fertilise it. With this technique, however, it’s possible that no spermatozoid is able to reach the inside of the egg in order to fertilise it. Therefore, there’s a greater risk of total fertilisation failure.
With the ICSI technique on the other hand, one spermatozoid is injected into the inside of the egg, meaning the risk of fertilisation failure is reduced.
The number of IVF-ICSI attempts necessary to achieve a pregnancy will depend on each patient’s particular case. There are some determining factors such as age, the number of mature eggs obtained and their quality, as well as the number of viable, transferrable embryos, among others.
However, according to data from the Spanish Fertility Society, 80% of patients become pregnant within 3 IVF-ICSI cycles. After 3 cycles, the recommendation is generally to substitute one of the gametes if a viable pregnancy has not been achieved. Normally patients are advised to consider using donor eggs.
Conventional IVF was developed as a treatment for cases of infertility related to tubal factors, endometriosis, unexplained infertility or failed artificial inseminations, among other reasons.
However, this technique cannot be utilised in cases of moderate or severe male factor infertility. Due to the high risk of fertilisation failure, conventional IVF is less commonly used than IVF-ICSI today.
The success of IVF-ICSI cycles may be negatively impacted by different factors involving both gametes. On the one hand, if the patient is over the age of 40 her egg quality may be impaired, and diminished egg quality negatively affects cycle results. On the other hand, fertilisation following ICSI may be less likely to successfully occur if the male’s sperm presents abnormalities such as severe oligozoospermia or asthenozoospermia, or in cases where a testicular biopsy is necessary in order to obtain spermatozoids.
